Modern Approach to Fibromyalgia Treatment: Evidence-Based Medicine
Fibromyalgia is one of the most mysterious diseases in modern medicine.
In this article
01 Inflammation as an etiological factor 02 Is there drug therapy? 03 What really helps? 04 Where science is heading 05 What this means in practiceFibromyalgia is one of the most enigmatic diseases encountered in modern medicine. The diagnosis is well-known, everyone knows something about it, and scientists’ opinions on the causes and mechanisms of fibromyalgia vary. Most likely, the reason for this confusion is that there isn’t one cause, but several. In this blog, we will gradually examine cause by cause and treatment methods. To find all articles about fibromyalgia, click on the “fibromyalgia” tag at the end of the article.
Science in the field of neuroplastic pain research is advancing very rapidly, with many studies. In this article, we will look at the evidence-based medicine’s approach to this disease as of March 2026.
01
Inflammation as one of the main etiological factors of fibromyalgia
The difficulty in diagnosing fibromyalgia lies in the absence of specific changes in the body’s anatomy or physiology that could be detected by conventional diagnostic methods – blood tests, radiological examinations.
The main problem with fibromyalgia is central sensitization: an increased sensitivity of the nervous system to pain signals.
But that’s not all.
In recent years, researchers have begun to look deeper and found that people with fibromyalgia have elevated pro-inflammatory markers in their blood, the very cytokines we are used to seeing in infections and autoimmune diseases. TNF-α, IL-6, IL-8 are consistently elevated in several independent meta-analyses. And PET scans of the brain show activation of microglia, immune defense cells located in nervous tissue.
🔥 Acute systemic inflammation
- High fever, redness, swelling
- CRP sharply elevated
- CBC altered
- Immediately visible – both in tests and clinically
🌫 Chronic neuroinflammation
- Quiet, localized, within nervous tissue
- Not accompanied by fever
- CRP may be slightly elevated or normal
- Standard tests do not detect it
02
Is there drug therapy for fibromyalgia?
We are used to the idea that if there is a disease, there must be a cure for it, but in this case, we are in for a disappointment.
Three drugs are approved for the treatment of fibromyalgia: duloxetine, milnacipran, and pregabalin. Sounds promising. But a large Cochrane review from 2025 yielded a sobering result: significant pain relief is achieved by approximately one in ten patients. And only for up to 12 weeks. After six months, there is no evidence of efficacy at all.
Nonsteroidal anti-inflammatory drugs – ibuprofen, naproxen, and others – do not work for fibromyalgia. At all. Their effect in randomized studies was no different from placebo. Which is logical: the inflammation here is not such that it can be simply “extinguished” by conventional means.
03
What really helps?
Data from many serious studies lead to unexpected results. The most convincing treatments turned out to be things not sold in pharmacies.
🏊 Movement
Meta-analyses show that physical exercise improves pain with an effect size of 72% to 96% – these are significant figures. Aerobic exercises combined with stretching, aquatic activities, Pilates, strength training – all of this works. Moreover, it works not only on pain but also on sleep, fatigue, and depression. The only condition: start slowly and increase gradually, always under the supervision of a specialist who understands chronic pain treatment. A sudden start leads to exacerbation.
🧠 Psychotherapy
Cognitive-behavioral therapy and hypnosis for fibromyalgia have high-quality evidence. The PROSPER-FM clinical trial from 2024 showed that psychotherapy led to improvement in 71% of participants versus 22% in the control group. It is important to understand that the effect of psychotherapy does not mean that the disease is not real and “it’s all in your head.” This is an absolutely scientifically proven mechanism: psychotherapy changes the way the brain processes pain signals.
Nutrition is one of the key modulators of neuroinflammation. Food affects the state of the central nervous system both directly, through the immune-boosting or immune-suppressing effects of food components, and indirectly, through changes in intestinal permeability, influence on the microbiome, and activation of peripheral inflammatory processes. The quality, composition, and timing of food intake shape immune responses, affect the activity of specialized immune cells of the nervous system, and alter the CNS’s vulnerability to inflammatory processes.
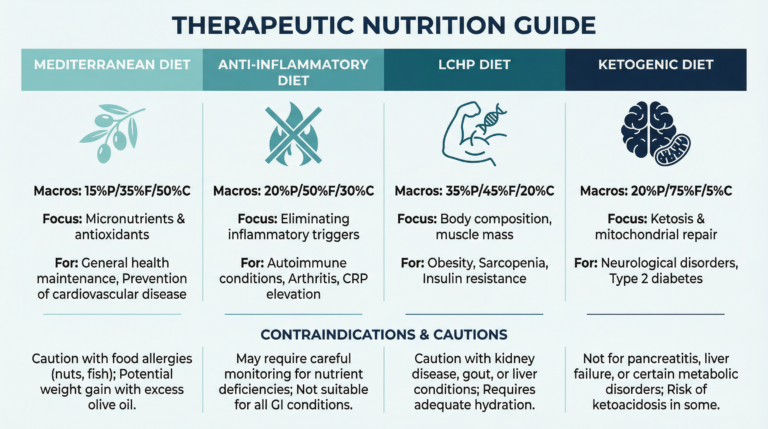
A Mediterranean diet, rich in antioxidants and omega-3 fatty acids, is associated with improvements in chronic pain, fatigue, and cognitive symptoms. A 2025 study indicates that reducing caffeine intake and a low-glycemic index diet may influence inflammatory pathways associated with fibromyalgia.
Add
- Fatty fish, omega-3
- Extra virgin olive oil
- Turmeric + black pepper
- Vegetables of all colors of the rainbow
- Berries and dark fruits
- Nuts, especially walnuts
- Green tea, garlic, ginger
Reduce
- Sugar and sugary drinks
- White flour and pastries
- Trans fats and margarine
- Ultra-processed foods
- Vegetable oils (omega-6)
- Excess caffeine
- Alcohol
04
Where science is heading
The most interesting developments, perhaps, are happening at the intersection of immunology and neurology.
Researchers have found that mast cells, small immune “capsules” in tissues, may play a role in neurogenic inflammation in fibromyalgia. Neuropeptides, such as substance P and corticotropin-releasing hormone, are elevated in patients and can trigger an inflammatory cascade precisely through them.
Another direction is specialized pro-resolving mediators (SPMs). These are substances that the body produces itself to “turn off” inflammation when the acute need for it passes. In fibromyalgia, this mechanism may malfunction. In animal experiments, SPMs have already shown the ability to alleviate chronic pain. This is a very promising direction in theoretical research, but it will be many years before its efficacy in humans is proven. In the meantime, we can use this knowledge to stimulate the body’s production of SPMs through diet: increase omega-3 intake, add regular physical activity, and adhere to an anti-inflammatory diet.
Natural SPM enhancers
2025 studies: active compounds in St. John’s wort and magnolia enhance SPM formation.
Physical activity
More than 150 minutes of moderate exercise per week increases SPM production.
Quitting smoking
Critically important: smoking increases pro-inflammatory markers and reduces anti-inflammatory agents.
Gut and brain
Growing evidence links fibromyalgia to dysbiosis. The “gut-immunity-brain” axis is a key player.
05
What this means in practice
For fibromyalgia patients and their loved ones, it is important to understand what is happening in the body with this disease.
This pain is real. Its mechanisms are complex but real. The absence of inflammation in tests does not mean that there is no inflammation. It simply means that ordinary tests do not detect it.
Medications can help manage symptoms during the acute phase, but they should not be expected to solve the underlying problem. The main work happens elsewhere: movement, sleep, nutrition, psychotherapy, and, crucially, understanding one’s condition.