Chronic Pain Is Always Linked to Inflammation, Even When Blood Tests Are Normal
Chronic pain is always linked to inflammation, even if blood tests don’t confirm it
Chronic pain without inflammation is like a fire without smoke. Theoretically possible. In practice, almost never.
01 Familiar story: pain is present, no diagnosis
When I explain to my patients that one of the causes of pain chronification is inflammation, I am often asked to order blood tests to confirm or refute this suspicion.
And often we see slightly elevated inflammation marker levels in the tests. But not always.
The fact is these tests show systemic inflammation markers. And inflammation related to chronic pain does not always affect them.
02 Inflammation in chronic pain
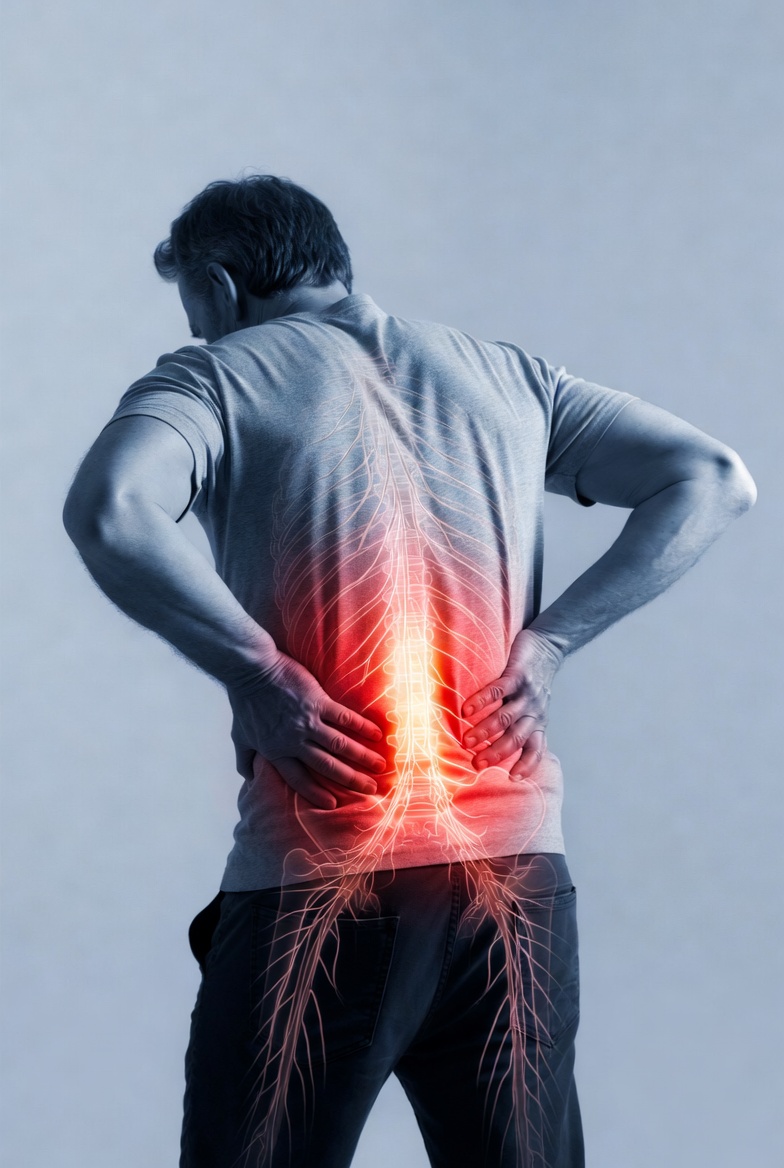
Pain is the result of an inflammatory process at the level of nervous tissue. When pain receptors are activated, they release inflammatory substances. When the nervous system is chronically activated, it itself becomes a source of inflammation.
This is called neuroinflammation — inflammation within the nervous system. It fundamentally differs from inflammation in, say, tonsillitis or arthritis. It is quiet, localized, chronic, and very poorly visible from the outside.
Acute systemic inflammation
High temperature, redness, swelling. CRP sharply elevated. CBC altered. Visible immediately — both in tests and clinically.
In chronic pain, we deal with the second type. Inflammatory cytokines, signaling molecules that trigger and sustain inflammation, are present in nervous tissue, spinal cord, brain, but are not detected in routine blood tests.
03 Why tests don’t detect it
Imagine a small but constant fire burning in the basement of one building in your city. Citywide smoke detectors placed throughout the city detect nothing because the smoke disperses before reaching them. That doesn’t mean there is no fire.
This is roughly how neuroinflammation behaves in relation to standard blood tests.
Blood-brain barrier
The brain and spinal cord are separated from the bloodstream by a special barrier. Inflammatory molecules from nervous tissue hardly enter the blood, so blood tests don’t detect them.
Low concentrations
Neuroinflammation is not at a level where cytokines “spill over” into the bloodstream. Their concentrations in blood are minimal, below the sensitivity threshold of standard tests.
CRP — marker of systemic inflammation
C-reactive protein responds to inflammation in internal organs and body tissues. In neuroinflammation, it may be slightly elevated in some patients. But normal CRP does not exclude neuroinflammation.
Specific markers are needed
Neuroinflammation can be detected by cerebrospinal fluid analysis, specialized markers (IL-6, TNF-α, IL-1β), or neuroimaging. These are not routine tests.
04 CRP and other markers: what real statistics show
In patients with fibromyalgia, chronic back pain, neuropathic pain, a slight increase in CRP and other inflammatory markers is found in a significant portion of patients. Doctors often consider this “clinically insignificant.”
But “clinically insignificant” does not mean “doesn’t matter.” Even mild chronic inflammation is a constant background noise that sustains pain sensitivity, disrupts sleep, and affects mood and cognitive functions.
📌 Important to understand: normal CRP does not mean “no inflammation.” It means “no systemic acute inflammation detected.” This is a fundamental difference. In chronic pain, we work with inflammation regardless of what the test shows.
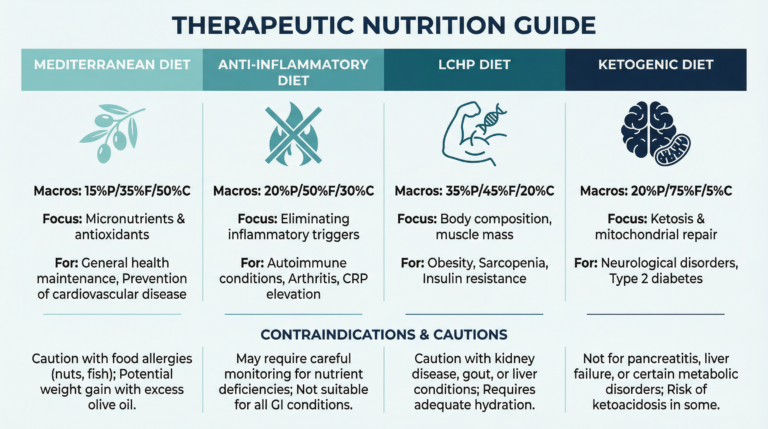
05 Anti-inflammatory diet
Nutrition is one of the most powerful yet accessible tools for managing inflammation. Inflammation literally feeds on what we eat.
Ultra-processed foods, excess sugar, omega-6 fats from vegetable oils support an inflammatory background. But there are foods that reduce this background.
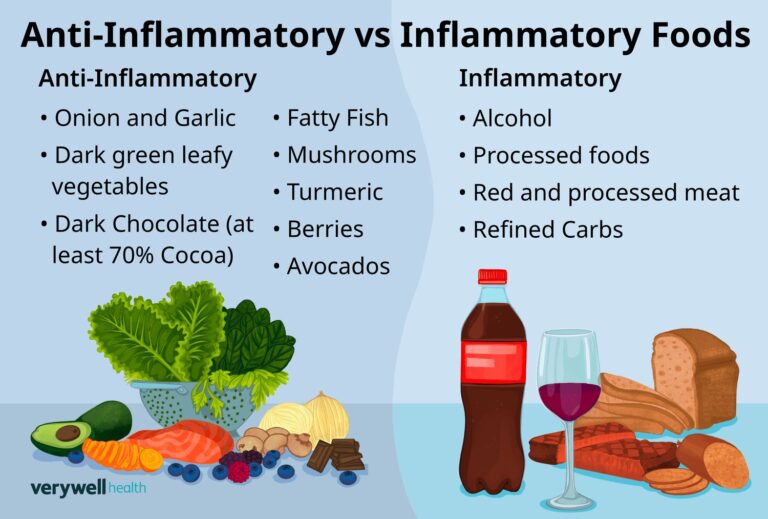
Add
- Fatty fish (salmon, sardines, mackerel)
- Extra virgin olive oil
- Turmeric + black pepper
- Vegetables of all rainbow colors
- Berries and dark fruits
- Nuts, especially walnuts
- Green tea
- Garlic and ginger
Reduce
- Sugar and sweet drinks
- White flour and baked goods
- Trans fats and margarine
- Ultra-processed foods
- Vegetable oils (sunflower, corn)
- Alcohol
- Red meat in large amounts
Detailed information on how nutrition works as a therapeutic tool for chronic pain is in the book “Nutrition as a Therapeutic Tool”. Practical principles, meal plans, and analysis of specific foods.
06 Naturopathic agents against inflammation
Good news: nature offers several very convincing anti-inflammatory agents. With real evidence base — not at the level of “neighbor’s grandma’s recipes,” but at the level of clinical studies.
Curcumin
The active substance in turmeric. Blocks several inflammatory pathways simultaneously, including NF-κB — the main “switch” of inflammation. Important: bioavailability is low, piperine (black pepper) or special forms are needed.
Omega-3 (EPA and DHA)
Fatty acids from fish oil — direct precursors of anti-inflammatory mediators. Reduce levels of inflammatory cytokines. One of the most studied natural agents.
Magnesium
Magnesium deficiency is one of the most common and underestimated factors of chronic inflammation. Magnesium participates in regulation of pain receptors (NMDA) and reduces neuroexcitability.
Vitamin D
Vitamin D deficiency is associated with chronic pain and enhanced inflammatory response. Vitamin D regulates the immune system and reduces production of pro-inflammatory cytokines.
Boswellia (frankincense)
Extract of boswellia resin is a potent inhibitor of the 5-LOX enzyme involved in the inflammatory cascade. Well studied in osteoarthritis and inflammatory bowel diseases.
EGCG (green tea)
Epigallocatechin gallate — the main polyphenol of green tea. A powerful antioxidant with anti-inflammatory properties. Reduces levels of TNF-α and IL-6 — key inflammatory cytokines.
⚠️ Important disclaimer: discuss any supplement intake with your doctor. Curcumin, for example, interacts with anticoagulants. Omega-3 in high doses thins the blood. Details matter.
Summary
Chronic pain is linked to a special type of inflammation — chronic neuroinflammation. It is difficult to detect with standard blood tests.
Correcting this inflammation requires a special anti-inflammatory diet, naturopathic, and sometimes medicinal treatment.
It is very important that this treatment is prescribed by a competent specialist. Self-treatment is dangerous.